By:
Published Date
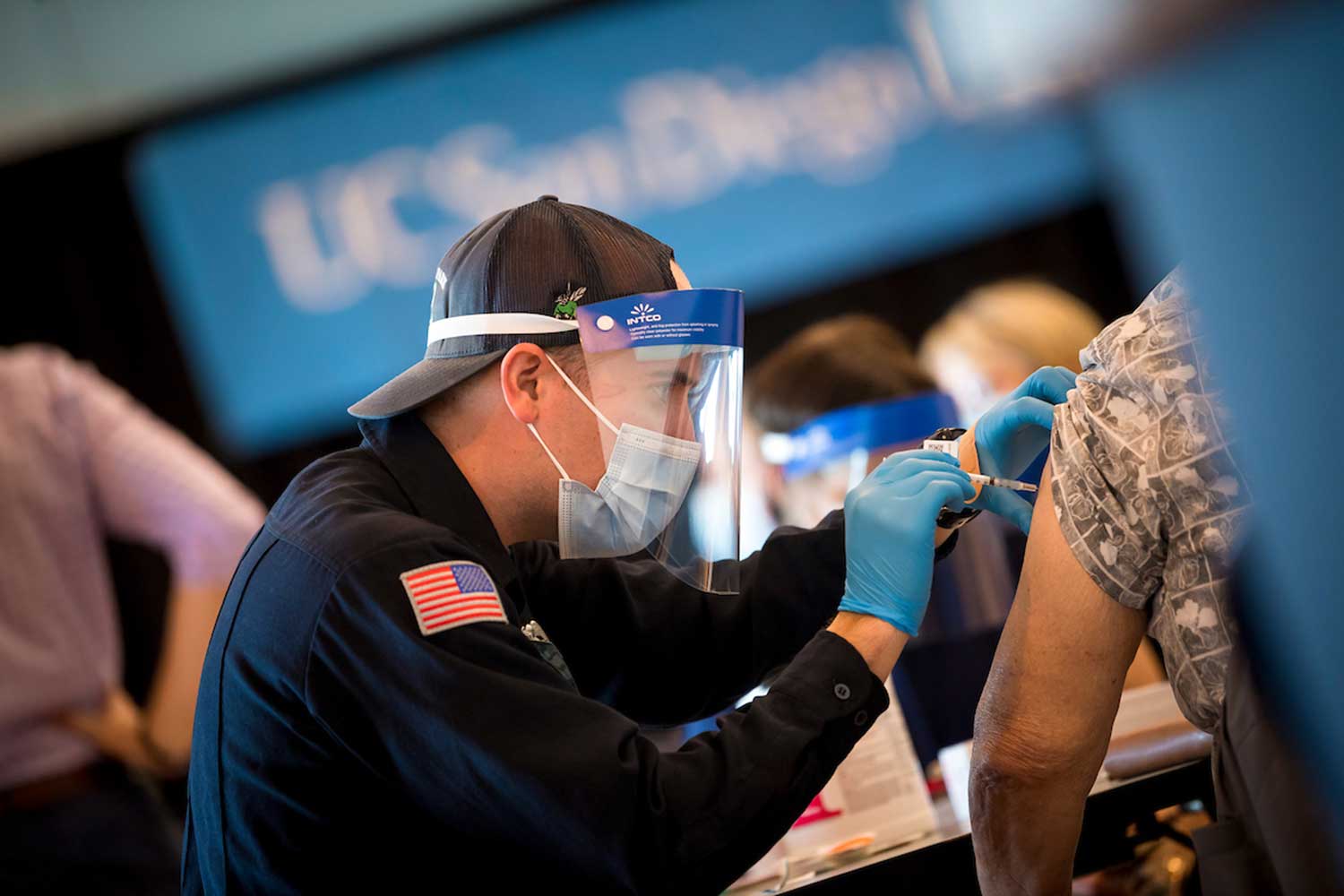
Q&A: Are COVID-19 Vaccines Safe and Effective?

Nearly one year ago, on March 13, 2020, San Diego County issued a two-week stay-at-home order to slow the spread of the COVID-19 pandemic. The gravity of the situation was growing quickly. Within nine months, the first vaccines were offered to health care workers, an incredibly quick timeline for vaccine development (most require five to 10 years). Now, over 635,000 residents of San Diego County have received their first COVID-19 vaccine dose.
Though vaccines are often in headlines and pop up in conversation, many people are still interested in learning more about how they function. Are they safe and effective? How do they work and are there potential side effects? What should I do after being vaccinated? To address these important topics and more, we spoke with Dr. Robert “Chip” Schooley, professor in the Department of Medicine at UC San Diego School of Medicine. Schooley is also a leader of UC San Diego’s Return to Learn program.
Q. Why is it important to be vaccinated?
A. COVID-19 vaccinations are an important way to protect yourself and your family. In the short term, you can keep those who are older and who have other underlying conditions from becoming severely ill and potentially hospitalized.
In the longer term, vaccines reduce viral replication in the community. The more people who become infected, the greater the risk of additional variants developing. And variants can weaken the strength of vaccines, resulting in a need for constant updates and refinements. It is critical to prevent the virus from spreading and replicating in the first place.
Q. How do the vaccines work?
A. Right now, two types of vaccines are available: those that use messenger RNA (mRNA) and ones that use a modified adenovirus to present the viral spike protein to the immune system. The goal of vaccination is to familiarize the immune system with the spike protein of the virus so that when someone is exposed, the person’s immune response can evolve much more quickly and gain control of the virus before severe illness develops. The Moderna and Pfizer vaccines use synthetic mRNA to instruct muscle cells to make the viral spike protein.
Vaccines that use mRNA are remarkably safe; mRNA has been termed the “instruction set for life.” It is used regularly to instruct every cell in our body on which proteins to make. They are produced in the nucleus of the cell by being copied from your DNA. They then go out into the main part of the cell where proteins are made and tell the cell’s protein production machinery what proteins to make. Once the instructions are read, the mRNA decays and its pieces are recycled to the nucleus to make new mRNA. The mRNA vaccines work the same way. The mRNA in these vaccines tell your muscle cells to make the viral spike protein. Once these instructions are delivered, the mRNA is degraded over 12 hours, and the spike protein that is created as a preview for the immune system disappears over 48 hours.
The Janssen (Johnson & Johnson) vaccine that was reviewed by the FDA on Feb. 27 uses a modified adenovirus that can enter cells but can’t replicate inside them or cause illness. The adenovirus carries instructions to the cell nucleus to make mRNA, encoding the viral spike protein. As in the case of mRNA vaccines in which the mRNA is directly delivered, the adenovirus vaccine-associated mRNA migrates out of the nucleus and tells the cell to make the viral spike protein. The adenovirus used in these vaccines is defective and cannot grow further. It is quickly degraded and disappears.
Q. Can you tell us more about the new Janssen (Johnson & Johnson) vaccine?
A. It is expected that 20 million doses of the Janssen (Johnson & Johnson) vaccine will be available in the U.S. by the end of March. This vaccine is slightly less effective than others in preventing mild disease but is very effective in preventing severe disease or death. The studies of this vaccine were carried out in the U.S., Africa and Brazil where the new variant strains are circulating. Although some people became mildly ill, no one was hospitalized and there were no deaths.
The primary goal of vaccinations is to avert hospitalization and any more deaths while we continue to decrease the amount of virus circulating. The Janssen vaccine prevents people from developing severe disease and death. There will eventually be a booster shot available like the other vaccines. For now, because the Janssen vaccine requires only one dose, we can get a large number of people vaccinated very quickly.
Q. Can the mRNA in vaccines alter your DNA?
A. Rumors have circulated that mRNA vaccines can change your DNA. This is false. Every cell in our body uses mRNA as a way to instruct cells on which proteins to make. While they enter cells to conduct their work, they do not enter the nucleus where DNA is stored. The vaccines that use mRNA to instruct cells to build the coronavirus spike protein help prepare your body to produce antibodies that combat coronavirus if you come in contact with it later. The mRNA is quickly degraded once it is in the body, which is one reason why these vaccines must be carefully preserved at very low temperatures.
Q. Are there any side effects?
A. Soreness in the arm at the site of the shot is common. After the second vaccination, because your immune system has already seen it once, you may have a more vigorous response. Some people have a low-grade fever or feel tired for about 36 hours, but serious side effects have been extremely rare. Others don’t experience any symptoms at all. Regardless, these are mild side effects that are certainly less concerning than the prospect of becoming infected with COVID-19.
Q. Are the vaccines effective against the new variants?
A. Moderna and Pfizer vaccines are 95% effective against the original variants and at least 90% effective against the new variants. Again, they will prevent the development of severe disease and hospitalization, even with new variants. The newly approved vaccines are slightly less effective with the variants, but still protect against severe disease and death.
Q. What happens if I don’t get my second dose within the recommended timeframe?
A. The two-vaccine sequence is a classic way to develop very high levels of immunity and it is important to get both doses. The first dose gives the immune system a first look at the harmful virus we need protection from. The second dose, or booster shot, causes the immune system to get really irritated when it appears again, resulting in the development of very high levels of antibodies. This is called a memory response, which can happen as soon as three weeks after the first vaccination. In fact, most two-shot vaccines are spaced at longer intervals than three to four weeks. For as long as six months after the first vaccination, a second shot can induce a vigorous booster response. Thus, even if your second dose is delayed for as long as two to three months, the booster response is extremely strong.
The only reason the vaccines were distributed three or four weeks apart in the initial clinical trials was to get as many people vaccinated as fast as possible. However, there is no evidence that you don’t get the same amount of memory response if the vaccines are given up to two to three months late. I recommend people receive both vaccinations because the memory response is the one that really solidifies the immunity that protects you for a long time.
Q. Why is it recommended to continue to mask and distance after vaccination? Is it possible to still be contagious?
A. We have learned through studies that some people who were infected before they were vaccinated continue to have viral shedding for the first couple of weeks after they are vaccinated. Then as their immunity rises from the vaccination, lower levels of virus are shed. There is good emerging evidence that vaccines decrease the rate of transmission; people aren’t prevented from shedding the virus, they just shed less. Although we recommend that all people continue to wear masks in public, those who have been vaccinated can mingle with others who have been vaccinated in small groups without masks, according to new guidance from the CDC. It is important to realize that full vaccine protection does not develop until two weeks have passed after the final vaccine dose and immunity should not be assumed until that time.
The other reason we recommend that everyone mask is that when you go into a grocery store, you want to see everyone masked. You can’t tell whether they have been vaccinated or not. By keeping everyone masked right now, it protects vulnerable people who have not been vaccinated and reinforces safe behaviors.
Q. How do you define vaccination success?
A. Vaccine success is defined as a person’s immune system effectively identifying and wiping out the virus before it causes any disease. While very few vaccines completely prevent people from getting infected, the primary goal is to prevent severe disease, hospitalization and death. In some people, particularly if they have been vaccinated a long time ago or they get a strain that is slightly less related to the vaccine strain, they can end up with a flu-like symptoms. However, it is still extremely rare for them to develop severe illness.
Q. Can a person be vaccinated if they are currently infected or had COVID-19 in the past?
A. There is no evidence that being vaccinated while you have COVID-19 (whether symptomatic or asymptomatic) is harmful. In fact, this happened in the vaccine trials and these individuals did not experience any side effects that differed from others.
For those who have recovered from COVID-19, it is still recommended that you are vaccinated. The reason is that vaccines induce better immunity than the real disease by two or fourfold. The vaccine may also offer stronger protection for a longer period and to a greater degree. There are also studies now emerging that suggest those who have been recently infected (within the past year) may need only a single vaccination since the illness itself has already familiarized the immune response with the virus. The initial vaccination in these people then essentially becomes the booster shot.
Q. How does the timeline of the COVID-19 vaccine development compare to others?
A. This is probably the fastest vaccine development in history. It was prioritized and accelerated because of the urgency of the epidemic. It is important to note that everything that would normally have been done was done with these vaccines—no steps were skipped.
The normal process would involve a small study to determine whether to move forward with the vaccine. After a lengthy analysis of perhaps a year, a second study would investigate the dosage and types of immune responses of the vaccine. Another year may pass before a larger study would commence to examine whether the vaccine prevents people from getting sick. Eventually the potential vaccine would be presented to the FDA, which would assess the safety and effectiveness of the vaccine. If the FDA approves a vaccine, then manufacturers gear up to produce the vaccine. The whole process can take five to 10 years.
The COVID-19 vaccines were developed within a very compressed timeline and many of the studies overlapped each other to accelerate the process. Manufacturers also had a purchase guarantee by the government, so the market was secured, and they actually had produced large amounts of vaccine before the vaccines were approved. These pre-produced vaccine doses were available the day the vaccines were approved which is why we were able to hit the ground running once the research studies were completed and fully reviewed.
Share This:
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.



