
State’s Stem Cell Agency Awards $18.2 Million Grant for B Cell Cancer Clinical Trial
UC San Diego researchers will combine an experimental drug with an approved drug in effort to boost remission rates and long-term cancer control
Published Date
By:
- Scott LaFee
Share This:
Article Content
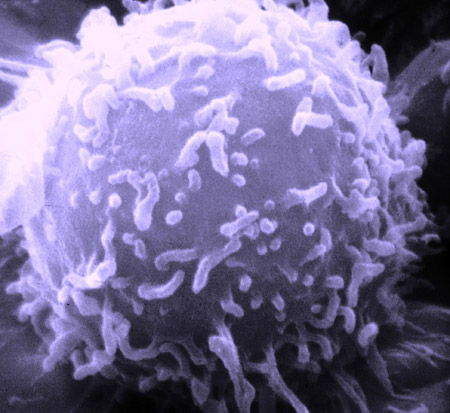
Scanning electron micrograph of B lymphocyte. Image courtesy of National Cancer Institute.
The Independent Citizens Oversight Committee of the California Institute for Regenerative Medicine (CIRM) today unanimously approved an $18.29 million grant to University of California San Diego School of Medicine researchers to fund a phase Ib/IIa clinical trial of a novel combination drug therapy for B-cell cancers.
The approach combines an experimental monoclonal antibody-based drug called cirmtuzumab with ibrutinib, a small molecule drug that inhibits a protein called Bruton’s tyrosine kinase. Ibrutinib, marketed as Imbruvica, is already approved to treat B cell cancers, like chronic lymphocytic leukemia (CLL) and mantle cell lymphoma (MCL). Cirmtuzumab targets ROR1, a cell surface protein present on tumors but not in normal adult tissues — a distinction that makes it an attractive target for anticancer therapy. Cirmtuzumab is currently in clinical trials for the treatment of CLL.
The new combined drug trial, intended to study both safety and efficacy, is headed by Thomas Kipps, MD, PhD, Distinguished Professor of Medicine and deputy director of research at UC San Diego Moores Cancer Center, in collaboration with colleagues at the UC San Diego CIRM Alpha Stem Cell Clinic — the cell therapy arm of the Sanford Stem Cell Clinical Center at UC San Diego Health.
“We are very excited about evaluating this combination of targeted therapies in the clinic,” said Kipps. “Although ibrutinib has been approved for treatment of patients with CLL or MCL, it is exceptionally rare for this drug by itself to get rid of all the leukemia cells or cause long-lasting remissions without continuous therapy.
“As a result, patients are recommended to take ibrutinib indefinitely — until they develop intolerance or resistance to this drug. By blocking a survival/growth-stimulating pathway that provides a lifeline to the leukemia cells of patients taking ibrutinib, cirmtuzumab can work together with ibrutinib to potentially kill all the leukemia cells, allowing patients to achieve a complete remission and stop therapy altogether.”
Kipps noted, too that cirmtuzumab targets cancer stem cells, which behave somewhat like the roots of the disease, resisting many forms of treatment and allowing a malignancy to grow back after apparently successful therapy. By targeting cancer stem cells, said Kipps, “cirmtuzumab may improve our capacity to achieve more complete and longer lasting remissions when used in combination with targeted drugs, such as ibrutinib, or other anti-cancer drugs for the treatment of patients with many different types of cancer.”
B cell malignancies are cancers of the blood. B cells are a type of white blood cell or lymphocyte, part of the immune system. Some B cells produce antibodies to immediately help fight off infections while others, called memory B cells, “remember” the pathogen in case of future infections. In B cell cancers, mutated B cells dysfunction or grow in an uncontrolled manner, resulting in diseases like CLL (the most common type of leukemia) and most non-Hodgkin’s lymphomas.
Cirmtuzumab was developed in Kipps’ laboratory under the auspices of CIRM’s HALT leukemia grant awarded to Dennis Carson, MD, principal investigator, and Catriona Jamieson, MD, PhD, deputy director of the Sanford Stem Cell Clinical Center and director of stem cell research at Moores Cancer Center. Kipps led one of the six projects, generating antibodies against ROR1 that, ultimately, led to the cirmtuzumab trials in patients with CLL.
“Every year around 20,000 Americans are diagnosed with CLL,” said Maria Millan, MD, interim president and CEO of CIRM. “For those who have run out of treatment options, the only alternative is a bone marrow transplant. Since CLL afflicts individuals in their 70's who often have additional medical problems, bone marrow transplantation carries a higher risk of life-threatening complications. The combination approach of cirmtuzumab and Ibrutinib seeks to offer a less invasive and more effective alternative for these patients.”
Cirmtuzumab has also shown efficacy against solid tumors. A clinical trial is planned to test it, in combination with the drug paclitaxel, for treating metastatic breast cancer. That trial is not yet recruiting participants. Cirmtuzumab’s name is a nod to CIRM’s long-standing support and research funding.
CIRM was created in 2004 by California voters with $3 billion in funding support to accelerate stem cell research and treatments. Since 2004, UC San Diego researchers have received at least 96 CIRM awards, totaling more than $182 million.
Share This:
You May Also Like
Stay in the Know
Keep up with all the latest from UC San Diego. Subscribe to the newsletter today.


